Prostatitis occurs in two forms - acute and chronic. If acute inflammation is treated quickly with antibiotics, chronic prostatitis becomes a serious problem in older men, adversely affecting quality of life. Chronic prostatitis can be caused by both infection and overload in the pelvic organs. The disease requires long-term and complex treatment.
Classification of the disease
Chronic prostatitis in men is divided into two types - congestive (abacterial, congestion) and infectious.
Chronic congestive prostatitis is a consequence of impaired prostate trophism. The disease develops with heart failure or lack of regular sex life.
Chronic abacterial prostatitis is characterized by moderately severe symptoms and the absence of acute pain syndrome. When analyzed, no infectious agent is detected in prostate secretion, hence the disease is called bacterial.Chronic infectious prostatitis is a consequence of untreated bacterial inflammation. The disease begins in an acute form due to infection of the prostate gland. The disease becomes chronic due to lack of adequate and timely therapy. Chronic infectious prostatitis is characterized by periodic exacerbations.
Causes of chronic non-infectious prostatitis
Speaking of chronic prostatitis, we most often mean a non-infectious disease caused by overload in the pelvic organs. This is due to the violation of prostate trophism - blood circulation, lymph flow, leakage of prostate secretions.
This form of the disease is directly related to lifestyle and is considered a disease of office workers. The main reason for the development of congestive prostatitis is physical inactivity.
Among the factors that predispose to the development of congestive prostatitis, there are:

- sedentary work;
- lack of regular sports;
- unbalanced diet;
- mbipesha;
- bad habits;
- varicose veins;
- hemorrhoids;
- irregular sex life.
The disease develops against the background of any condition, accompanied by circulatory disorders in the lower extremities. Often, prostatitis occurs with overweight, when, as a result of increased stress in the lumbar region and lower limbs, metabolic processes in this area are disrupted.
If due to the peculiarities of the profession you have to sit all day, you should move at least in the evening.
Bad habits can cause prostatitis to develop. Smoking destroys blood vessels and disrupts normal blood flow. Due to the physiological characteristics of a person, it mainly affects the blood circulation of the lower extremities and the pelvic region.
Sex plays an important role in the functioning of the prostate gland. The optimal number of sexual intercourses per week for a man over 40 is 3-4. A smaller amount leads to a violation of the flow of prostate secretion, a larger amount - to the depletion of organs.
Another cause of congestive prostatitis is heart failure. This disease is characterized by impaired blood circulation, including the pelvic organs.
Reasons for developing chronic infectious prostatitis
Chronic bacterial prostatitis is a consequence of acute untreated inflammation of the prostate gland. This form of the disease is characterized by severe symptoms and the presence of pathogenic agents found in prostate secretion.
The most common causative agents of infectious prostatitis:
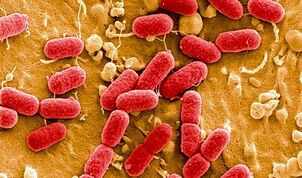
- E. coli and Pseudomonas aeruginosa;
- staphylococcus and streptococcus;
- chlamydia;
- ureaplasma;
- Trichomonas; Mushroom flora
- .
Infection enters the prostate gland in three ways: through the bloodstream, lymph, or through the urethra. The last route of penetration of pathogenic agents is valid in cases of infection with chlamydia, ureplasma or Trichomonas.
Reasons for developing the disease:
- reduced immunity;
- severe hypothermia;
- stress;
- long-term antibiotic therapy.
Pathogenic condition bacteria are always present in the body, and only strong immunity does not allow them to be activated.
Chronic bacterial prostatitis develops from an acute form in the following cases:
- presence of a chronic focus of infection;
- incorrectly selected antibiotic therapy;
- late completion of treatment;
- weakened immunity.
In most cases, the chronic form of the disease develops precisely because of improper treatment. This occurs when the antibiotic therapy regimen is not properly designed or self-medicated. Stopping antibiotics when you feel better results in the disease agent not being completely destroyed. Any decrease in immunity or hypothermia in this case leads to new development of the disease.
The most difficult to treat is fungal prostate caused by yeast-like fungi. This pathogen quickly develops resistance to antifungal drugs, which makes it difficult to treat and increases the risk of developing a chronic form of the disease.
Symptoms of the disease
In chronic prostatitis, the symptoms are mild, however, with a decline in immunity or after suffering stress, the disease worsens.
The most common symptoms of chronic prostatitis in men are:
- urinary disorder;
- heaviness in the prostate;
- weakening of potency;
- encouraging the night to use the toilet.
With a worsening of chronic prostatitis, pain is noticed in the bladder and perineum. The frequency of stimulation in the toilet can reach 10 per hour. At the same time, the flow of urine is weak, it is necessary to strain the muscles to urinate, but the process itself does not bring relief and repeated stimuli appear after a few minutes.
The symptoms and treatment of chronic prostatitis depend mainly on the form of inflammation. With congestive prostatitis, erection problems are common. This is due to impaired blood circulation. Ejaculation can occur quickly, or is absent altogether due to thickening of the prostate secretion.
With infectious inflammation of the prostate gland or chronic bacterial prostatitis, pain may occur when urinating and burning in the urethra after ejaculation. Such symptoms are accompanied by irritation of the urethral mucosa by disease-causing agents contained in prostate secretion.
Prostatitis and erectile dysfunction

Inflammation of the prostate is not visible to the eye, the symptoms of chronic prostatitis have no obvious manifestations, but refer to internal disorders. One of the characteristic symptoms of the disease is a weakening of the erection.
Erectile dysfunction in congestive prostatitis develops in several stages. The disease itself can continue for a long time without pronounced symptoms and the signs of prostatitis will appear only with a strong weakening of the immune system.
Abacterial inflammation of the prostate may be suspected by changes in erection. An increase in potency is observed at the beginning of the development of the disease. The husband wakes up quickly, but the ejaculation also comes quickly. This is due to a change in the secretion viscosity of the prostate gland. Discomfort may be felt during ejaculation, but pain is characteristic of infectious but not congestive prostatitis.
This causes a number of psychological problems that exacerbate the course of the disease. Erectile dysfunction due to problems with blood flow is exacerbated by the fear of a sexual partner, which can lead to the development of impotence on the background of prostatitis.
Urinary Disorder
Problems with urodynamics are seen in all forms of prostatitis.
Chronic abacterial inflammation is characterized by a nocturnal urge to urinate. It is caused by swelling of the prostate gland, which worsens at night. There is a weakening of urine pressure and the need to tense the pelvic floor muscles to urinate. At the same time, he feels heaviness and fullness in the bladder, and occasional spasms may appear. Due to the frequent desire to use the toilet at night, problems with sleep and insomnia appear. All this affects the psychological state of man and further aggravates the course of the disease, since against the background of stress there is a decrease in immunity and a slowdown of metabolic processes.
Men often complain of cramps in the lower abdomen, which is explained by the increased tone of the bladder muscles. Usually, severe symptoms of prostatitis are marked by a decline in immunity. Without an exacerbation of the disease, the pain syndrome may be completely absent.
Congestive prostatitis is characterized by severe prostate edema. The contours of the organ become blurred, the prostate itself swells and increases in size. In this case, there may be a feeling of fullness in the rectum and increased discomfort during bowel movements. Problems with urination are due to compression of the urethra by the swollen prostate gland.
Why is prostatitis dangerous?

The consequences of chronic prostatitis depend on several factors:
- age of patient;
- severity of symptoms;
- current duration;
- effectiveness of drug therapy.
The longer a man lives with a chronic prostate, the more severe the consequences of the disease. In most cases, the urinary system is affected. With bacterial prostatitis, kidney infection can occur when urine returns. This is due to the entry of pathogens into the urethra during ejaculation.
Constant irritation of the bladder and urethra can lead to inflammation. Against the background of prostatitis, cystitis and urethritis of various natures are often diagnosed.
In chronic prostatitis, the consequences affect the psycho-emotional state of the man. Violation of potency, frequent desire to use the toilet, discomfort in the bladder - all this leads to the development of stress. Prostatitis can be an indirect cause of neurosis and depression.
Disruption of the nervous system against the background of constant disturbance in the genitourinary organs leads to a decrease in immunity and deterioration of all metabolic processes in the body. Thus, prostatitis provokes nervous disorders, which worsen the course of the disease and the circle is closed.
Persistent discomfort, impaired potency, inability to sleep - all of these greatly affect the quality of life.Disease Diagnosis
If inflammation of the prostate is suspected, a urologist or andrologist should be consulted. The following diagnostic methods are used to make a diagnosis:
- palpation of the prostate colon;
- Ultrasound and TRUS of an organ; renal ultrasound
- ;
- analysis of prostate secretion;
- PSA blood test.
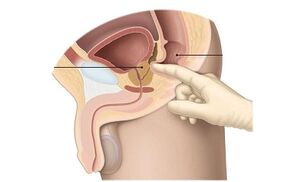
The need for further examinations is determined after palpation of the rectal organ. This procedure is also known as prostate massage. The doctor inserts two fingers into the opening of the rectum and feels the prostate. Inflammation is evidenced by a change in organ structure, heterogeneity of prostate tissue and contours. During the massage, the organ is stimulated and the prostate secretion is secreted by the urethra. It is collected for further analysis. Prostate secretion analysis shows:
- amount of lecine grains;
- leukocyte and erythrocyte count;
- presence of pathogenic microorganisms;
- presence of fungal microflora.
This allows not only to determine the nature of the inflammatory process, but also to identify the pathogen in infectious prostatitis.
Ultrasound and TRUS are performed more to rule out prostate stones than to diagnose prostatitis, as the method is not very informative, compared to secretion analysis.
a PSA blood test is prescribed to rule out oncopathology in the prostate gland. Also detects inflammation or adenoma of the prostate. How to treat chronic prostatitis depends on the test results and the type of inflammation.
Treatment characteristics
Chronic prostatitis treatment regimen is a combination of medicines, physiotherapy and folk remedies. The treatment is complemented by a change in lifestyle - menu adjustment, giving up bad habits, regular sports and sex life.
It is important to understand that for chronic prostatitis, treatment will last at least six months. In addition to medications to relieve inflammation, men are prescribed long-term rehabilitation therapy, which is necessary to normalize the functioning of the prostate gland.
Medications
How to treat chronic prostatitis depends on the form of the disease. Medications for chronic prostatitis include:
- antibiotics or anti-inflammatory drugs;
- rectal suppositories to normalize trophism; Immunostimulants
- and general health-promoting agents.
Antibiotics are used to treat chronic prostatitis in men, but only if it is an infectious inflammation of the prostate. How to treat infectious prostatitis in men depends on the pathogen and the success of the previous therapeutic course. In acute bacterial inflammation, macrolide antibiotics are prescribed in most cases. They effectively suppress the activity of pathogens and have a wide spectrum of action. In case of non-compliance with the treatment regimen or improper choice of drugs, the microorganisms that caused the inflammation quickly develop resistance to macrolides, which greatly causes the disease to pass into a chronic form.
Fluoroquinolones are effective antibacterial agents for prostatitis caused by microorganisms. They have a pronounced anti-inflammatory activity against a wide range of pathogenic microorganisms. Despite the fact that fluoroquinolones have no natural analogues, which is the reason for the lack of resistance of pathogenic microorganisms to the action of the drug, it is necessary to carefully follow the treatment regimen chosen by the doctor. Otherwise, the drug will be ineffective and antibiotic therapy will have to be repeated.
Antibacterial drugs and tablets are not used to treat chronic non-infectious prostatitis. With congestive prostatitis, inflammation is not caused by germs but by a trophism disorder, so it is inappropriate to use antibiotics for treatment. They use anti-inflammatory drugs instead. They are applied in short courses to reduce inflammation and swelling. The drug is prescribed in suppositories or injections. Treatment lasts an average of one week, the drug is administered rectally at night or intramuscularly once a day. With severe inflammation, it is possible to use the medicine twice a day.
Anti-inflammatory drugs are not antibiotics. The tablets are successfully used to ease the inflammatory process with non-infectious or congestive prostate. On average, doctors prescribe two pills a day for 5 days, and then transfer the patient to phytopreparation therapy that improves prostate trophism.
In case of severe urinary disorders, treatment is supplemented with alpha-blocking group drugs. These medications relax the bladder, reducing muscle tone, allowing urine to flow normally. Medications in this group are taken one tablet per day in short courses, treatment with alpha-blockers rarely exceeds one week.
Once the inflammation has subsided, congestive (infectious) and infectious prostatitis is treated with medications that normalize prostate gland trophism. Medications contribute to:
- reduce inflammation;
- pain syndrome relief;
- normalization of urination;
- increase potency.
For chronic prostatitis, these drugs are used for at least two weeks. They come in the form of rectal suppositories. The recommended dose is one candle daily at night.
Propolis suppositories are recommended to restore local immunity. They relieve inflammation, improve blood circulation and the release of prostate secretions, and also significantly increase immunity, preventing prostate deterioration. The medication comes in the form of small suppositories that are injected into the rectum at night.
Furthermore, your doctor may recommend ichthyol suppositories. They relieve inflammation and reduce swelling of the prostate gland.
Preparations based on echinacea extract are recommended as a general tonic for prostatitis. They strengthen the immune system and prevent the development of prostate exacerbations. With the appearance of neuroses and insomnia on the background of prostatitis, the doctor may recommend sedatives.
Physiotherapy for chronic prostatitis
The causes of chronic prostatitis lie in poor circulation to the pelvic organs. To accelerate the recovery and restoration of prostate trophism, physiotherapy methods are widely used:
- magnetic therapy;
- electrophoresis;
- shock wave therapy;
- acupuncture.
There are many methods of home physiotherapy. The most popular are special devices. They create alternating magnetic fields that have a positive effect on metabolic processes, eliminating congestion in the pelvic organs.
Darsonvalization can also be used at home. This is a micro current effect that improves metabolic processes. You can buy home treatment equipment at any medical device store, but it is recommended that you consult your doctor first.
Prostate massage is used to treat congestive prostatitis. It is performed by a specialist in a medical institution. Organ stimulation allows you to get rid of edema and discomfort, and also facilitates stagnant secretion of the prostate. The course of treatment consists of 10-15 procedures.
Folk remedies
Whether chronic prostatitis is treated depends on the range of therapeutic measures taken. Traditional medicine will help complement the medication treatment.

Home-made suppositories are used to relieve inflammation in the prostate. To prepare candles, you will need 200 g of each fat base, 40 ml of propolis extract. The base is melted in a water bath, propolis is poured slowly into it, stirring constantly. When the product acquires a uniform color, it is poured into food film and packaged in the shape of a sausage. The mass should be refrigerated for one hour to cool. When the product has cooled, it is cut with a knife into equal pieces in the form of torpedoes, approximately 5 cm long and 2 cm in diameter. These candles should be stored individually wrapped in the refrigerator. The recommended dose is a suppository in the rectum opening before bedtime. The duration of treatment is 2-3 weeks.
You can also make candles with pumpkin seed oil and honey. Dimensions are 200 g base, 50 ml oil and 3 tablespoons honey. As a base, you can take beeswax, lanolin, cocoa butter. Such suppositories relieve inflammation, improve prostate function, and increase immunity.
To treat chronic prostatitis at home, you can use various infusions and decoctions. One of the most effective remedies is parsley juice. 3 tablespoons should be taken daily.
Traditional medicine recommends consuming 30 g of pumpkin seeds every day. They contain many nutrients that are necessary for the normal functioning of the prostate gland.
Another effective treatment is a mixture of pumpkin seeds, nuts and honey. To prepare the medicine, you need to take 100 peeled seeds and the same number of walnut kernels, put them in a suitable container and pour 500 ml of honey. The product is kept in the refrigerator for 4 days to be filled and then 4 large spoons are taken every day.
Surgical Treatment
Whether chronic prostatitis can be cured permanently depends on the severity of the disease and the age of the patient. With frequent exacerbations, you need to take medication constantly.
Surgical treatment of prostatitis in most cases is not performed. Perhaps the use of radical measures - complete removal of the prostate gland. Such an operation is performed only if the prostate does not fulfill its functions due to chronic inflammation, and drug treatment is ineffective. Also, prostatectomy is practiced with the risk of developing oncology.
Interestingly, the effects of prostatitis are usually seen in old age, in men over 65 years old. This raises a number of treatment difficulties:- diseases of the cardiovascular system;
- contraindications for taking medication;
- many side effects.
Many men, who have suffered with prostate for more than 10 years, insist on surgery. This is usually accompanied by poor drug tolerance and a large number of side effects. Doctors say surgery is a last resort, and with the right approach, prostatitis can be cured by conservative methods.
Prevention and forecasting
Once we understand what chronic prostatitis is in men and how dangerous it is, the question immediately arises as to whether the disease can be completely cured.
Patient testimonials show that chronic prostatitis can be cured, but it will take a long time. The course of treatment lasts on average six months or more. Urologists agree that adequate therapy, lifestyle changes, and a balanced diet will help relieve inflammation.
Most often, recurrences and recurrent episodes of inflammation after prolonged remission are encountered by those men who do not follow the doctor's recommendations, but are treated on the advice of friends. Importers It is important to understand that success in treating therapy depends on correctly chosen drug therapy. Lead to worsening or re-manifestation of signs of chronic prostatitis may:
- taking unsystematic medications;
- non-compliance with doctor's recommendations;
- stop treatment after first improvement;
- bad habits;
- lack of physical activity.
Self-medication often leads to deteriorating well-being. This is especially true in cases of infectious inflammation, when the patient independently chooses antibiotics without testing.
A common mistake men make is to stop treatment when the first improvements appear. In this case, the inflammation does not go away, but only diminishes for a while. With a drop in immunity or hypothermia, the disease will be felt again.
In addition to medication, prostatitis requires lifestyle changes. It is important to give up bad habits, normalize your diet and start playing sports. With prostate, it is recommended to do yoga, exercise therapy, swimming. Any workout that involves the pelvis will benefit. Men with this condition, especially sedentary work, should do 10-minute exercises every day and do a full workout several times a week. Also, during the treatment of chronic prostatitis, it is necessary to have sex, as regular ejaculation helps reduce prostate edema.
The success of treating prostatitis depends on timely diagnosis, so if you notice problems with urination, you should consult a urologist as soon as possible.






























